How to Avoid Parasitic Echinococci That Infect the Liver, Lungs and Even the Brain
An echinococcus infection is caused by an approximately 5mm long parasite which can be caught by consuming parasite eggs found on berries and fruit from orchards or the forest, or by stroking dogs and cats, for example. Echinococcosis is a serious and usually incurable disease, where patients often have to take medication for the rest of their lives.
 Hepatologist Sniedze Laivacuma is an assistant at the Department of Infectology at the Faculty of Medicine at Rīga Stradiņš University (RSU). She has conducted a three-year-long study on echinococcosis. This is the first study on the prevalence, risk factors, diagnosis and treatment of this disease in Latvia. For many years, echinococcosis was thought not to be a problem in our country, but cases seem to be increasing every year.
Hepatologist Sniedze Laivacuma is an assistant at the Department of Infectology at the Faculty of Medicine at Rīga Stradiņš University (RSU). She has conducted a three-year-long study on echinococcosis. This is the first study on the prevalence, risk factors, diagnosis and treatment of this disease in Latvia. For many years, echinococcosis was thought not to be a problem in our country, but cases seem to be increasing every year.
What is echinococcosis?
Echinococcus is a parasite that humans can be intermediate hosts to. Carnivorous animals are definitive hosts of echinococci. The parasite attaches itself to the intestines of definitive hosts, while in intermediate hosts it can infect the liver, lungs, kidneys, spleen and even the brain and the bones. It lives and reproduces there.
People get infected with the parasites when they ingest their eggs. Most commonly this happens while eating fruit or berries from a forest or orchard, stroking a cat or a dog and failing to wash their hands afterwards. It is easy to get the infection, but the disease is not contagious and humans are not vectors for the disease.
Two types of echinococci can be found in Latvia – cystic and multilocular. Cystic echinoccoci reside in dogs’ intestinal tracts. It is most commonly found in dogs living on farms or in close proximity to forests. Multilocular echinococci are common in foxes, raccoons and other forest animals. In cystic echinococcosis empty cysts develop in the body of the host in which new parasites develop. With multilocular echinococcosis one cyst transforms into several smaller ones.
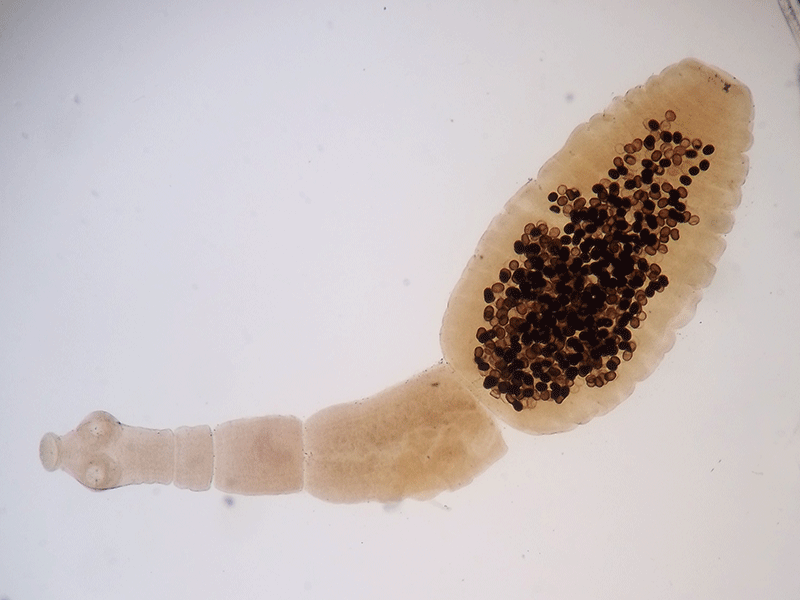
The adult echinococcus parasite is about 5 mm long and can lay more than 100,000 eggs. Source: https://commons.wikimedia.org
Does this mean that people can get infected by eating unwashed berries and failing to wash their hands with soap?
Yes, of course!
Why is the morbidity of echinococcosis on the rise in Latvia and worldwide?
A study of small household gardens was conducted in France, which has the highest incidence of echinococcosis in Europe, and echinococci eggs were found in almost every garden. This is because of the warm climate there as a result of which the eggs do not die during the winter. In addition, France has a flat terrain and many meadows inhabited by small rodents, so there are many foxes that infect the environment with faeces.
We are destroying the natural environment – cities are expanding closer to forests. Animals adapt to the new living conditions and come to farms and cities in the search of food. The media frequently publishes stories of foxes or other animals seen in the city or suburbs.
What are the symptoms of echinococcosis?
If a patient has had the disease for a long time they might have itchy skin as a result of the bile ducts being compressed by the parasite.
But in general patients with echinococcosis do not have any specific symptoms, therefore this disease is most frequently diagnosed by chance.
In the event of abdominal pain, or discomfort a patient might undergo abdominal ultrasound through which lesions in the liver might be detected. Additional examinations are then performed to diagnose the lesions as echinococci.
Can people become infected by eating game meat, or cow or pig liver from a relative’s farm?
People cannot become infected by eating meat. As I mentioned, people get infected with parasite eggs from the ground, or by stroking cats, dogs, or wild animals accustomed to humans that approach people looking for food.
How common is echinococcosis?
Incidence of echinococcosis in European countries fluctuates from 0.1 to 10 cases per 100,000 residents. The largest epicentre of this disease in Europe is Southern France and other southern countries. It must be kept in mind that Latvia is located next to Russia, Belarus and Poland where echinococcosis is quite common.
Since 1999, approximately 200 people have been infected with the disease in Latvia. Over the last years 10 to 15 new patients are diagnosed with echinococcosis every year and the number keeps growing.
Historically the distribution of echinococcosis in the North has been much lower compared to warmer countries or Asia, for instance. For years this disease was not common in Scandinavia or in the Baltic States considering the global context. There are one or two new cases per year in Estonia, compared to 10 to 15 cases in Latvia, and 30 to 50 cases in Lithuania. As you can see – the further south, the more common the disease.
As the global climate becomes warmer echinococci eggs can survive for longer in nature, even up to a year. If temperatures do not fall too low, even more eggs survive. In Latvia, we no longer experience the long, cold winters that we did in the past.
Are there any extensive studies on this disease in Latvia?
No studies on this disease, its risk factors, diagnosis or treatment have been carried out in Latvia so far. Therefore, the goal of my study was to detect the incidence of echinococcosis in our country, to identify risk factors and improve diagnostic and treatment strategies. To achieve this I collected and analysed the personal and medical data of over 100 patients. Another patient group of more than 100 respondents was surveyed to determine possible risk factors and detect immunogenetic risk factors, etc.
I took an interest in echinococcosis already when I was a medical student at RSU. I recall writing my first student-level research paper on this topic in 2010.
Echinococcosis was long not considered to be a problem in Latvia, that it does not affect us because of the small number of patients. Unfortunately, the facts now show the opposite.
What are the risk factors of contracting echinococcosis in Latvia?
In Latvia, people living in rural areas close to forests and wild animals are at higher risk of contracting echinococcosis. The risk increases if domestic animals like cats and dogs are kept on the farm because it is impossible to control where the cats and dogs wander and what they eat. Both dogs and cats eat mice that often get echinococcus eggs from foxes.
Slaughter practices on farms also play a role, as does hunting. There is a higher risk of infection in families where someone hunts and takes their dogs along. Dogs commonly eat the intestines of the game that contain parasites. Dogs are therefore at risk of becoming vectors of the disease.
What determines why one person contracts the disease, while another in similar circumstances stays healthy?
Many of us probably come into contact with parasite eggs on a daily basis, however not everyone becomes infected with the disease. This is, to a great extent, determined by genetic factors. The immune system plays a key role.
Besides, these are two species of the parasite and each species has several genotypes with distinctive features – some parasites are more dangerous, others most often infect the liver, etc. These variations are yet to be studied in Latvia and in Europe.
Is this disease treatable?
If the parasites are focused in one location in the body, then the disease can be treated surgically. If several organs are affected, however, patients will have to use antiparasitics for life since the recovery rate of these patients is low. The medications inhibit the parasites’ reproduction. They cannot, however, eliminate the parasites completely. Long-term use of the medication may lead to the parasites becoming dormant, or disappear as they fight the active substances of the medication. Most commonly, however, the parasites start reproducing as soon as the medication is halted.
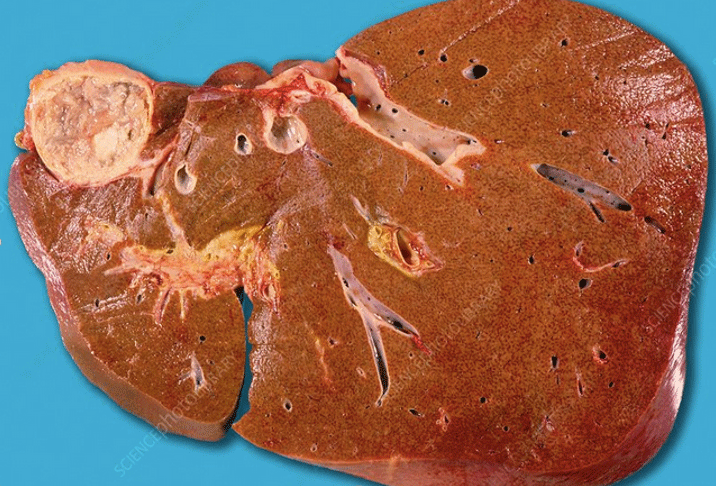
Echinococcal Cysts in the liver. Source: https://www.sciencephoto.com
There are no other, better therapy options available at present. Research into new potential medicines is currently being conducted in France, Germany, China and other Asian countries. Doctors are, therefore currently limited to the range of medications available at present.
Most cases of the disease are diagnosed when the disease has already taken hold. It is rare to diagnose echinococcosis in its initial stages when it could still relatively easily be surgically removed from the one location in the body where it has established itself.
Is it true that echinococcosis is compared to cancer? Why?
Yes. Multilocular echinococcosis spreads like a malignant tumour. It enters an organ, penetrates the walls of blood vessels and sends pieces into other organs that attach themselves to the walls there and start growing and reproducing – like cancer metastasis.
Can you die from echinococcosis?
Yes! When we had selected 116 patients to take part in the study sample and fill out a questionnaire, 31 of them had already died.
Why it is important to develop diagnostic methods for echinococcosis?
To make general practitioners and other physicians understand which of their patients could potentially have echinococcosis. This issue is, of course, sometimes addressed at medical conferences and in professional magazines, but we have to be more diligent about adopting general practices of what to do in cases when a lesion is detected in the liver. Patients need to be referred to get additional tests instead of dismissing cysts as something common and unremarkable. An attitude like this could result in the failure to diagnose a serious disease.
I have had patients with echinococcosis who have not visited their general practitioner for 20 years, and the echinococci have spread considerably during this time! It would be great if general practitioners in Latvia, like their colleagues abroad, kept an eye on their patients and called them to remind them to come for regular check-ups.
What are the most important conclusions of your study?
The most important conclusions concern establishing risk factors, including genetic risk factors, by analysing what determines whether a particular person might get infected or not, the severity of the disease, and what the best treatment course could be.
During the study I concluded that there are several risk factors in Latvia: living on a farm in a rural area, especially for longer periods of time; the presence of domestic animals on the farm; hunting; the presence of cats and dogs on the farm; cats and dogs living unattended and eating small rodents or the internal organs of slaughtered animals.
Outcomes from echinococcosis treatment improve if the treatment starts in the first year after diagnosis, if there has ever been a six-month treatment course, or if the treatment is repeated annually.
Doctors should follow specific treatment guidelines. This is necessary to avoid each doctor interpreting how long a patient should take specific medicines differently. It’s important to remember that the efficiency of treatment increases with the duration and number of treatments.
What would you recommend people do to protect themselves from contracting this disease?
There is no magic method for avoiding an echinococcosis infection. Wash your hands regularly and deworm your cats and dogs at least twice a year. Avoid eating berries without washing them first. I would recommend fencing off your vegetable and fruit gardens to limit wild animals accessing them.
And do not forget to go to your doctor for regular check-ups even if you feel well, especially if you live in a rural area and keep pets or other animals.
Facts about Sniedze Laivacuma:
- 2010: graduated from RSU (medical doctor’s diploma)
- 2012 – 2015: student at the RSU Department of Doctoral Studies
- Assistant at the Department of Infectology of the Faculty of Medicine
- Infectologist and hepatologist at Riga East Clinical University Hospital and ARS Health Centre
- Research work devoted to infectious diseases, parasitic diseases, viral hepatitis and echinococcosis
- Lecturer on infectious diseases and infectology at RSU
- Author or co-author of 16 scientific articles
Related news
 RSU Research Breakfast highlights new cooperation initiatives for developing Riga For RSU Employees, Research
RSU Research Breakfast highlights new cooperation initiatives for developing Riga For RSU Employees, Research