Scientists Study Innovative Cancer Treatment Methods
A team of scientists consisting of radiologists, nuclear medicine physicians, urologists, radiation therapists, oncologists, residents and students, have begun to implement the Fundamental and Applied Research Project ‘Impact of Targeted Molecular Imaging with FL-PSMA-1007 and 68Ga-PSMA-11 PET/CT in Multimodal Evaluation of Recurrent Prostate Cancer’. The title seems rather complex, but the purpose of the project is simple – to facilitate the development of prostate cancer treatment.
Knowing that only lung cancer affects more men than prostate cancer, it is clear why this study is so important. We asked Maija Radziņa, Head of the Rīga Stradiņš University (RSU) Radiology Research Laboratory, and the Project Manager and leading researcher, to tell us more about the nature of this innovative project.

How will this project help patients?
This nuanced study focuses more on diagnosing the recurrence of a tumour, rather than initial diagnosis. We are therefore dealing with patients who have already received serious treatment for prostate cancer, but where there are indications that cancer has returned. This is called cancer recurrence.
We are currently using a specific substance, fluorine 18, to which we add another substance - prostate-specific membrane antigen (PSMA).
This compound attaches to prostate cancer cells in the human body. So, if cancer is radically and fully removed, there should not be any cancer cells. However, if some cells remain, prostate-specific antigen (PSA) levels in the blood rise and activity occurs on a cell level.
Through imaging we can tell the exact location of this activity – it might occur in a lymph node, in the same spot as the first oncological process, or cancer might have spread to the bones or other parts of the body.
What are the advantages of this method?
The greatest advantage of this method is that you do not have to look for cancer in separate parts of the body: the substance, which is injected in the vein, shows us several activity spots at the same time.
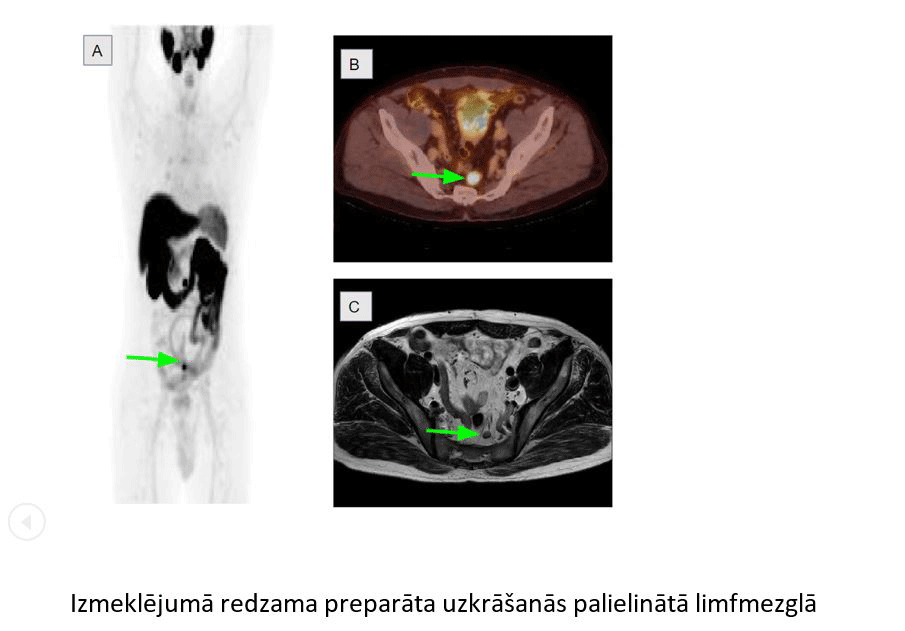
Accumulation of substance in an enlarged lymph node
When a patient arrives for a test, we inject the radioactive substance and wait until it accumulates in the sick cells, if there are any. Then we register the spots of radioactivity in the patient’s body with a special scanner and later we can project these spots as images on a screen. As a result, we get an abstract image with bright spots which we can merge or connect with an image of computed tomography and be able to tell if changes have occurred in a particular bone, or a lymph node. In addition, we perform magnetic resonance tests as the second diagnostic method. Then we compare the two methods.
The more progress we make, the more convinced we are that both methods are necessary. The method of administering radioactive substances is the best for detecting relapses in lymph nodes, whereas magnetic resonance shows local relapse locations where cancer has already been operated on.
What should be done after cancer cells have been detected?
This method enables us to detect and destroy cancer cells. The procedure for destroying cells is similar. A radioactive substance is administered, it reaches the particular cell and creates a small spot of radiation. Thus, a person does not need to undergo extensive radiation therapy or chemotherapy. In comparison to other methods, this procedure is milder on the body.
Nuclear medicine is very interesting because it is constantly developing. Science centres are constantly testing new combinations, new compounds. The method of administrating a radioactive compound is already being used in diagnostics in Europe and worldwide. Practice shows that after the initial cancer treatment, patients spend several years in remission, but later the overall defence capacity of a body might fall, and the faulty cell might become active again. Therefore, it is very important to undergo regular blood tests to see the dynamics of the prostate specific antigen.

Tell us about your team.
This is a multidisciplinary study. Radiologists cannot conduct a study like this without cooperation partners - urologists, oncologists, radiation therapists and other colleagues. First, a urologist decides if specific tests are necessary and performs a surgery. Sometimes surgery is required, sometimes radiotherapy, at other times a combination of both. Nowadays, the course and tactics of treating oncological patients is determined by a medical council that consists of urologists, oncologists, radiologists and radiation therapists. This is very important because initial treatment can have an impact on the future life quality of a patient.
Our team consists of Assoc. Prof. Egils Vjaters, Head of the Urology Clinic of Pauls Stradiņš Clinical University Hospital, experienced nuclear medicine specialists, like Lilita Roznere, who has been working at the RSU Nuclear Medicine Clinic for a long time examining patients and doing research work. Radiologist Māra Tirāne, who has long experience in diagnosing prostate cancer, radiology resident Laura Saule, who has a keen interest in oncoradiology and nuclear medicine. My role as a project manager is to organise and coordinate the process between RSU and other institutions, for example, the medical centre ARS. In addition to my administrative duties, I interpret and analyse the test results. In general, it can be said that urologists from all over Latvia are involved: we have patients from Riga East Clinical University Hospital, Pauls Stradiņš Clinical University Hospital, Vidzeme Hospital, Liepaja Regional Hospital, Riga 1st hospital. This is a large-scale project.
Some people manage to recover from cancer or prevent cancer from recurring, others do not. Why is this?
This is determined by cell aggression. Initial radiation is important - the greater the dose of radiation, the higher the chances of cancer not coming back. This is observed in 5 - 40% of cases. In addition, nowadays prostate cancer affects not only men in their eighties, but younger men as well.
The innovative substance that we are using in our project is not yet widely used in treatment, but results are very promising, and we hope that the results will make a significant contribution to the treatment of this serious disease.